Carpal Tunnel Syndrome: Symptoms, Causes, and Treatment Options in Granite City, IL
When the median nerve is squeezed within the carpal tunnel, symptoms of carpal tunnel syndrome can begin. Symptoms often include tingling, numbness, pain, or weakness that may seem minor early on but grow more disruptive over time.
If your goal is to manage symptoms while continuing to work and enjoy daily life in Granite City, IL, hand therapy is frequently a practical place to begin. Care guided by experienced Granite City, IL physical therapists through Axes often focuses on getting people back to normal routines safely and confidently.
If you’re ready to move forward, you can connect with a nearby Axes location, schedule an appointment online, or stop by one of our locations for a complimentary injury screening.
Quick Summary
- This condition involves compression of the median nerve in the wrist, which can result in changes in sensation, pain, and hand weakness.
- Symptoms often worsen at night and usually affect the thumb through part of the ring finger, while the little finger is typically spared.
- Symptoms are often influenced by repetitive activity, prolonged wrist positioning, swelling, and certain medical conditions.
- Diagnosis is based on symptoms, physical exam findings, and sometimes nerve testing to confirm nerve compression.
- Non-surgical treatment is frequently successful, particularly when symptoms are addressed early with splinting, activity changes, and therapy.
- Delaying treatment may allow symptoms to advance and increase the risk of permanent nerve changes and hand weakness.
An Overview of Carpal Tunnel Syndrome
At the wrist, the carpal tunnel forms a tight space that structures must pass through. The structure is bordered by wrist bones on the bottom and sides, with the transverse carpal ligament spanning across the top. Passing through this space is the median nerve, which originates in the neck and travels down the arm into the hand.
Increases in pressure inside the carpal tunnel, whether from swelling or other changes, can place stress on the median nerve. This often leads to sensory changes such as tingling or numbness, along with weakness during gripping, pinching, or precise hand movements.
Common Symptoms of Carpal Tunnel Syndrome
Carpal tunnel syndrome doesn’t always announce itself with a big dramatic pain spike. A lot of people notice a pattern first:
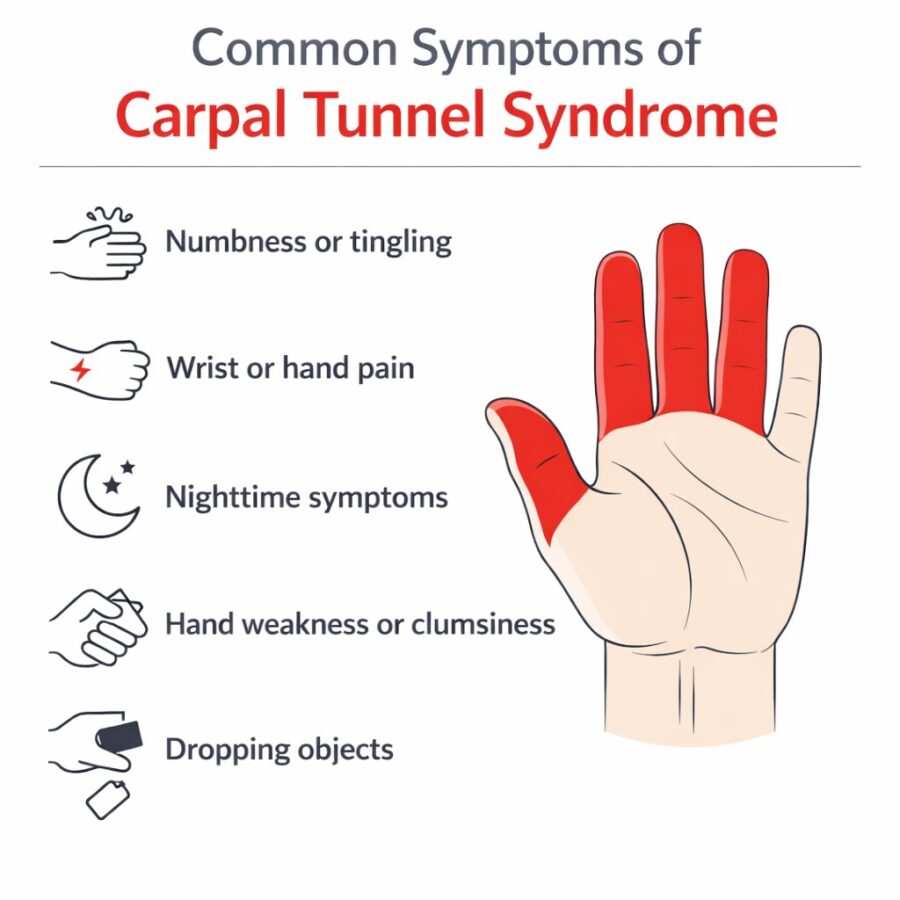
Common symptoms of carpal tunnel syndrome include:
- Altered sensation such as numbness or tingling in the thumb through part of the ring finger
- Burning, aching, or electric-like sensations in the hand or wrist
- Pain or tingling that occurs at night and disrupts sleep
- Feeling the need to shake or move the hand to relieve numbness
- Hand weakness or clumsiness, especially with gripping or fine motor tasks like buttoning clothing, holding keys, writing, or using tools
- Increased tendency to drop items
- Pain that feels like it’s coming from deep within the wrist or hand and may sometimes travel up the forearm
Recognizable symptom patterns
In addition to the symptoms themselves, clinicians often look for specific patterns that suggest carpal tunnel syndrome:
- Symptoms that are worse overnight or apparent early in the morning
- Numbness or tingling during sustained gripping or static wrist positions, such as holding a phone, reading a newspaper, or gripping a steering wheel
- Symptoms that briefly improve when activity stops or the wrist position changes
An important finger pattern clue
Paying attention to which fingers are involved can provide helpful diagnostic clues. The median nerve does not supply sensation to the little finger, so carpal tunnel symptoms usually spare the pinky. If numbness or tingling consistently involves the little finger, it may point toward a different nerve or another cause of hand symptoms.
What Contributes to Carpal Tunnel Syndrome?
The cause is often multifactorial rather than a single issue. Symptoms usually develop as pressure accumulates within the tight carpal tunnel space.
Common contributors include:
Repetitive and prolonged wrist or hand use
Activities that involve repetitive motions, prolonged gripping, tool use, or awkward wrist positions can increase symptoms, particularly when breaks are limited.
Inflammation-related pressure
Increased wrist swelling from injury or overuse can narrow the carpal tunnel and place added pressure on the median nerve. Because the carpal tunnel is such a confined space, even mild inflammation can increase pressure, making rest, ice, and splinting helpful early on.
Anatomy and structural changes
Some people have a naturally narrower tunnel, and changes from arthritis or wrist trauma can alter the space over time.
Medical and lifestyle risk factors
Some health conditions are linked to increased carpal tunnel risk, including rheumatoid arthritis, diabetes, hypothyroidism, and obesity.
Pregnancy-related changes can trigger symptoms that usually improve after childbirth but may still indicate increased long-term risk.
Lifestyle factors such as smoking, heavy alcohol use, and poor nutrition may also play a role.
Diagnosing Carpal Tunnel Syndrome with Granite City, IL Physical Therapists
A diagnosis is often reached through a detailed symptom discussion and physical exam, with further testing considered in certain cases.
Why symptom patterns matter
Diagnosis often begins by reviewing the symptom patterns described above, particularly nighttime symptoms and numbness that occurs with sustained wrist positions or prolonged gripping.
Common in-office tests used during diagnosis
During evaluation, therapists may use hands-on testing to determine whether wrist positioning or gentle pressure reproduces carpal tunnel symptoms.
- Phalen’s test – placing the wrist into flexion to assess whether tingling or numbness appears in the fingers
- Tinel’s sign – lightly tapping over the median nerve to see if tingling or electrical sensations travel into the hand
- Strength testing – checking grip strength and median nerve–related muscle function
- Sensation testing – checking for reduced or altered feeling in the fingers commonly affected by carpal tunnel syndrome
Symptom patterns and exam findings are interpreted together to determine if median nerve compression is present.
When imaging or nerve tests are used
In some situations, additional testing may be recommended based on symptoms and exam findings, including:
- X-rays – used to look for bone or joint issues such as arthritis or prior fracture; they are not used to diagnose carpal tunnel syndrome itself
- Ultrasound – allows visualization of nerve size and surrounding structures at the wrist
- Nerve conduction studies and electromyography (EMG) – used to evaluate how well the median nerve and affected muscles are functioning and to help distinguish carpal tunnel syndrome from other nerve conditions
Electrodiagnostic testing is often considered the most definitive way to confirm median nerve compression when the diagnosis is unclear or symptoms are more advanced.
Managing Carpal Tunnel Syndrome at Home in Granite City, IL
In Granite City, IL, treatment for carpal tunnel syndrome usually begins with conservative care. The focus is simple—decrease irritation to the median nerve, settle symptoms, and address contributing factors.
What you can do right away (mild symptoms)
For early or mild symptoms, short-term home strategies may reduce irritation, including:
- Resting from aggravating activities
- Using cold packs for short intervals throughout the day
- Considering NSAIDs for pain/swelling relief
- Using a wrist splint to limit pressure on the median nerve
Basic adjustments early on may help reduce irritation and swelling.
How Granite City, IL Physical Therapy Treats Carpal Tunnel Syndrome
While splints and activity advice can be useful, most cases require a more comprehensive plan. That’s where Granite City, IL physical therapy and hand therapy come in.
A good PT/hand therapy program in Granite City, IL often focuses on:
- Limiting ongoing nerve irritation
- Restoring wrist and forearm movement and strength
- Addressing posture and movement patterns upstream (yes, even the shoulder/neck can matter for how your arm loads)
- Allowing you to stay active and productive with less stress on the wrist
What therapy may include
No two carpal tunnel treatment plans are exactly the same. Treatment is adjusted based on symptoms, daily demands, and how the wrist and hand respond over time. Treatment may involve several of the following components.
1) Symptom-calming strategies
Initial sessions aim to calm symptoms and reduce stress on the median nerve. This phase isn’t about pushing through pain or trying to fix everything at once.
Common examples include:
- Education on night splinting to maintain neutral wrist positioning
- Adjusting task duration or frequency to limit irritation
- Short-term adjustments to reduce strain during work, driving, or daily tasks
- Selective use of taping techniques to support the wrist during activity
The goal is to calm symptoms without requiring you to completely stop normal activities.
2) Mobility and movement of tendons and nerves
Mobility work looks at movement quality throughout the wrist, forearm, fingers, and surrounding tissues, rather than focusing only on the nerve. Restrictions or stiffness anywhere along the arm can increase stress at the wrist and play a role in symptom development.
Treatment may include:
- Joint mobility techniques for the wrist and forearm to improve flexion, extension, and rotation
- Soft tissue techniques aimed at reducing forearm muscle stiffness, including manual therapy and instrument assisted soft tissue mobilization when appropriate
- Mobility work for the fingers and thumb to reduce stiffness or guarding
- Tendon and nerve gliding exercises used on a case-by-case basis, such as:
- Tendon gliding: structured finger movement patterns designed to improve how flexor tendons move within the carpal tunnel
- Median nerve gliding: controlled movements designed to improve nerve mobility and reduce sensitivity
- In some cases, trigger point dry needling may be used to address forearm muscle tension that contributes to wrist and hand strain
Improving mobility throughout the arm can reduce excess strain at the wrist and support more efficient movement. Tendon and nerve gliding are integrated carefully alongside other interventions.
3) Strength, endurance, and functional training
Strength training involves far more than simple grip tools. The goal is to prepare the hand and wrist for everyday tasks.
This may include:
- Building grip and pinch strength in a controlled, progressive manner
- Endurance-focused exercises to prepare for prolonged hand use, including typing or tool work
- Functional strengthening, including lifting, carrying, pushing, or pulling tasks that mimic work or daily demands
- Exercises that build tolerance to load across different wrist positions
Treatment focuses on returning to normal activities while keeping symptoms controlled.
4) Practical ergonomics that reduce strain
Simply telling someone to “sit up straight” isn’t an effective solution. Effective ergonomics looks at how small changes can reduce wrist and hand strain.
Examples may include:
- Adjusting keyboard, mouse, or tool positioning so the wrist stays closer to neutral
- Reducing grip force demands during work or daily tasks
- Changing task setup, height, or sequencing to limit prolonged wrist strain
Small adjustments can significantly reduce pressure on the median nerve over the course of a day. When symptoms are work-related, work rehabilitation programs and functional capacity evaluations may assist with return-to-work planning.
5) Therapeutic ultrasound when indicated
Ultrasound is sometimes used as an adjunct to other treatment strategies. Ultrasound parameters are adjusted to match individual needs. Ultrasound is combined with other treatment strategies rather than used on its own.
6) Pre- and post-surgical rehabilitation (when needed)
In cases where surgery or injections are involved, rehabilitation before and after the procedure can help improve outcomes and functional recovery.
Physical Therapy Care for Carpal Tunnel Syndrome in Granite City, IL
Axes Physical Therapy provides patient-focused care in Granite City, IL through licensed physical and occupational therapists. With an average of 15+ years of experience, our Granite City, IL physical therapists also provide specialized hand therapy services, including treatment from Certified Hand Therapists (CHTs) for complex hand and wrist conditions like carpal tunnel syndrome.
If symptoms are starting to interfere with sleep, work, or everyday activities you don’t usually think twice about—like opening jars, gripping the steering wheel, texting, or lifting—it’s a good time to get a plan.
Book an evaluation with Axes Physical Therapy in Granite City, IL to better understand your symptoms and create a treatment plan tailored to your needs. Get started by calling the nearest Axes location, scheduling online, or visiting any clinic for a free injury screening.
Common Questions About Carpal Tunnel Syndrome Treatment in Granite City, IL
Does typing always lead to carpal tunnel syndrome?
No. Repetitive hand use like typing can play a role, but carpal tunnel syndrome is usually multifactorial, involving anatomy, inflammation, wrist posture, and certain health conditions.
What makes carpal tunnel syndrome worse during sleep?
Nighttime flare-ups often occur because wrist posture and fluid changes increase pressure in the carpal tunnel. Night splinting helps maintain a neutral wrist position and may relieve nighttime symptoms.
How can providers tell if symptoms are carpal tunnel syndrome?
Diagnosis is based on your symptom pattern, physical exam findings, and, when needed, additional testing such as nerve conduction studies or EMG to confirm nerve compression or rule out other causes.
Is physical therapy effective for carpal tunnel syndrome?
Physical therapy is frequently part of early treatment and can include movement work, strengthening, ergonomic changes, and symptom management strategies.
When might steroid injections be used?
Corticosteroid injections may be considered when symptoms don’t improve with other conservative care and short-term pain relief is needed to reduce inflammation and nerve irritation.
When should surgery be considered for carpal tunnel syndrome?
Surgery is generally reserved for cases where symptoms do not improve with conservative treatment or nerve injury risk is present.



















































































































































































