Carpal Tunnel Syndrome: Symptoms, Causes, and Treatment Options in Winfield, MO
Carpal tunnel syndrome develops as the median nerve becomes irritated within the tight passageway at the wrist. Symptoms often include tingling, numbness, pain, or weakness that may seem minor early on but grow more disruptive over time.
When symptoms start interfering with everyday activities, many people in Winfield, MO look for a conservative place to begin, specialized hand therapy services can be an effective first step. Care guided by licensed physical therapists serving Winfield, MO with Axes Physical Therapy often focuses on getting people back to normal routines safely and confidently.
Taking the next step doesn’t have to be complicated. you can contact the Axes location nearest you, schedule an appointment online, or stop by one of our locations to take advantage of a complimentary injury screening.
Quick Summary
- This condition involves compression of the median nerve in the wrist, which can result in changes in sensation, pain, and hand weakness.
- Many people notice symptoms are worse at night and primarily involve the thumb, index, middle, and part of the ring finger, with the pinky usually unaffected.
- Symptoms are often influenced by repetitive activity, prolonged wrist positioning, swelling, and certain medical conditions.
- Diagnosing carpal tunnel syndrome typically involves reviewing symptoms, performing a physical exam, and occasionally using nerve testing.
- Conservative treatment is often effective, especially when started early, and may include activity modification, night splinting, and physical or hand therapy.
- Delaying treatment may allow symptoms to advance and increase the risk of permanent nerve changes and hand weakness.
An Overview of Carpal Tunnel Syndrome
The wrist contains a narrow space known as the carpal tunnel. The “floor” and sides are formed by the small wrist bones, and the “roof” is a strong band of tissue called the transverse carpal ligament. Running from the neck through the arm and forearm, the median nerve passes through the carpal tunnel on its way into the hand.
Increases in pressure inside the carpal tunnel, whether from swelling or other changes, can place stress on the median nerve. These changes can show up as numbness, tingling, or weakness that affects grip, pinch strength, and fine motor control.
Common Symptoms of Carpal Tunnel Syndrome
Carpal tunnel syndrome doesn’t always begin with intense or sudden pain. For many, symptoms follow recognizable patterns early on.
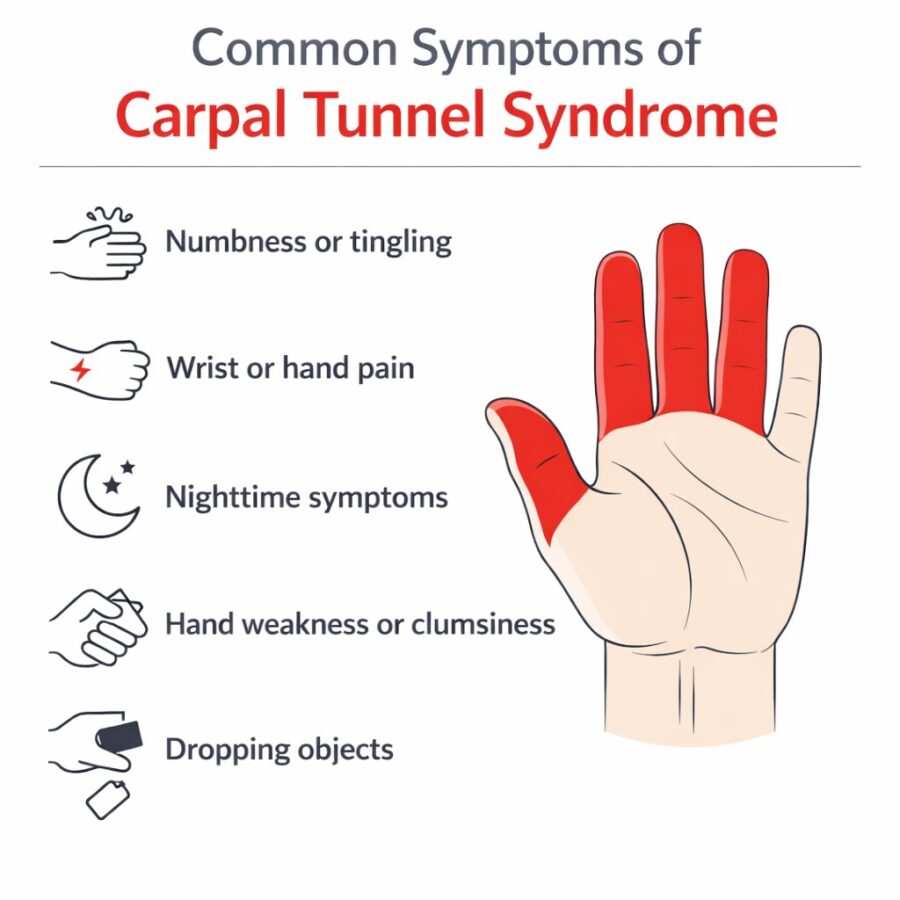
Common carpal tunnel syndrome symptoms include:
- Numbness or tingling in the thumb, index finger, middle finger, and often part of the ring finger
- Uncomfortable sensations such as burning or electric-like pain in the wrist or hand
- Nighttime symptoms, such as pain or tingling that wakes you from sleep
- A need to shake the hand out to “wake it up” or relieve numbness
- Hand weakness or clumsiness, especially with gripping or fine motor tasks like buttoning clothing, holding keys, writing, or using tools
- Increased tendency to drop items
- Pain that feels like it’s coming from deep within the wrist or hand and may sometimes travel up the forearm
Common symptom patterns
Symptoms alone don’t tell the whole story, so clinicians also look for patterns that help identify carpal tunnel syndrome:
- Symptoms that are worse overnight or apparent early in the morning
- Tingling or numbness that appears during prolonged gripping or when the wrist is held in one position, like holding a phone or steering wheel
- Symptoms that briefly improve when activity stops or the wrist position changes
A helpful “finger map” clue
Paying attention to which fingers are involved can provide helpful diagnostic clues. The little finger is usually unaffected in carpal tunnel syndrome since it is not supplied by the median nerve. When the pinky is involved, it can indicate that something other than carpal tunnel syndrome is contributing to symptoms.
Common Causes of Carpal Tunnel Syndrome
The cause is often multifactorial rather than a single issue. Instead of a sudden injury, pressure tends to increase slowly over time in the carpal tunnel.
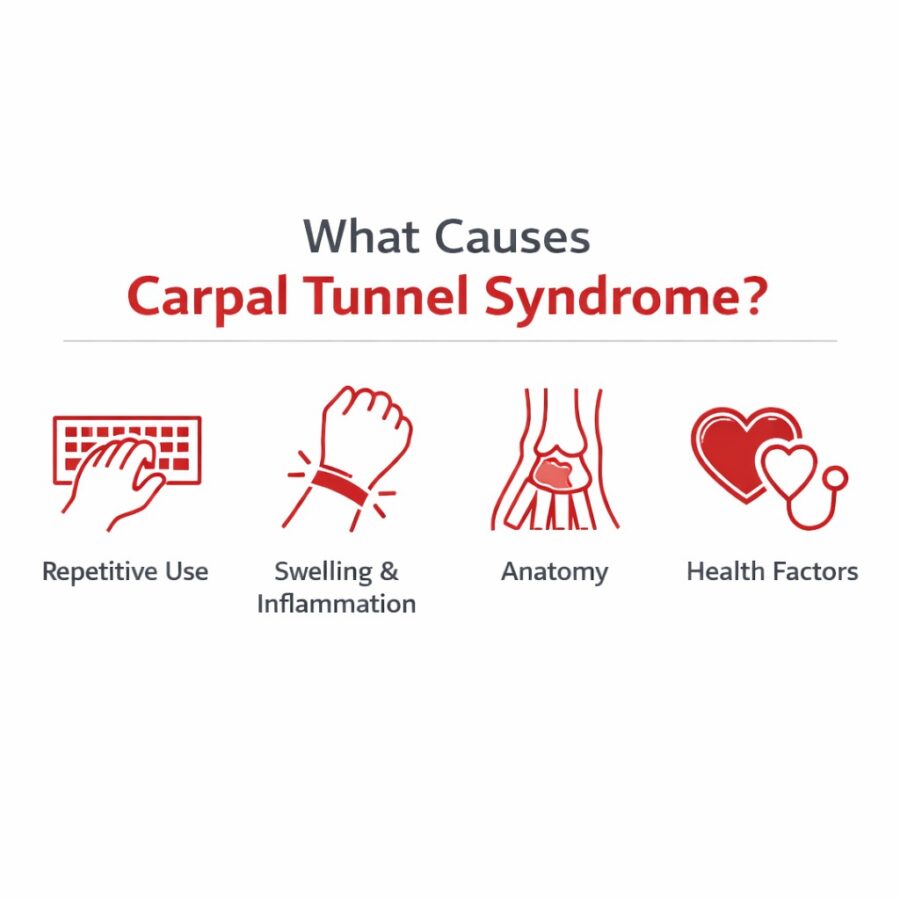
Some of the most common contributors include:
Repetitive or sustained wrist/hand demands
Activities that involve repetitive motions, prolonged gripping, tool use, or awkward wrist positions can increase symptoms, particularly when breaks are limited.
Wrist swelling and inflammation
Increased wrist swelling from injury or overuse can narrow the carpal tunnel and place added pressure on the median nerve. Small changes in swelling can significantly affect pressure inside the tunnel, which is why early symptom management strategies can be effective.
Anatomical contributors
Natural differences in wrist anatomy, along with changes from arthritis or previous injury, can affect the size of the carpal tunnel.
Health and lifestyle factors
Certain medical conditions are associated with higher CTS risk (for example: rheumatoid arthritis, diabetes, hypothyroidism, obesity).
Fluid shifts during pregnancy can contribute to symptoms, which frequently resolve postpartum but may recur in the future.
Smoking, excessive alcohol use, and poor diets can also contribute to the condition.
How Carpal Tunnel Syndrome Is Diagnosed by Winfield, MO Physical Therapists
Diagnosis is usually a combination of your symptom story and a physical exam, sometimes with additional testing.
Why symptom patterns matter
Diagnosis often begins by reviewing the symptom patterns described above, particularly nighttime symptoms and numbness that occurs with sustained wrist positions or prolonged gripping.
Common in-office tests used during diagnosis
Physical examination often includes simple tests that assess whether specific wrist positions or light pressure bring on symptoms related to median nerve compression.
- Phalen’s test – holding the wrist in a flexed position to see if numbness or tingling develops in the fingers
- Tinel’s sign – tapping along the median nerve at the wrist to assess for tingling or shock-like sensations
- Strength testing – checking grip strength and median nerve–related muscle function
- Sensation testing – assessing sensation changes in the fingers typically involved in carpal tunnel syndrome
Results from testing are combined with reported symptoms to help confirm whether the median nerve is under pressure.
When additional testing may be needed
Depending on your case, your Winfield, MO physical therapist may also recommend or request:
- X-rays – helpful for identifying structural issues but not for confirming carpal tunnel syndrome itself
- Ultrasound – allows visualization of nerve size and surrounding structures at the wrist
- Nerve conduction studies and electromyography (EMG) – used to assess nerve signal transmission and muscle function to confirm median nerve involvement or rule out other causes
When symptoms are more severe or diagnosis remains uncertain, electrodiagnostic testing is commonly used to confirm median nerve compression.
Managing Carpal Tunnel Syndrome at Home in Winfield, MO
Carpal tunnel care in Winfield, MO often starts with non-invasive approaches. The goal is to calm symptoms, reduce median nerve pressure, and address underlying contributors.
Immediate at-home steps for mild symptoms
Stanford suggests that if symptoms are mild, a short window of home care (1–2 weeks) may relieve symptoms, including:
- Resting from aggravating activities
- Using cold packs for short intervals throughout the day
- Using NSAIDs to help manage pain or inflammation
- Wearing a wrist splint to reduce pressure on the median nerve
Basic adjustments early on may help reduce irritation and swelling.
How Winfield, MO Physical Therapy Treats Carpal Tunnel Syndrome
Basic strategies alone aren’t always enough—addressing why the nerve is irritated is key. That’s where physical therapy and hand therapy in Winfield, MO play an important role.
A comprehensive hand therapy program in Winfield, MO may focus on:
- Limiting ongoing nerve irritation
- Improving wrist/forearm mobility and strength
- Addressing posture and movement patterns upstream (yes, even the shoulder/neck can matter for how your arm loads)
- Helping you keep doing your job and daily tasks with less strain
What therapy may include
No two carpal tunnel treatment plans are exactly the same. Plans are modified over time depending on symptom response and functional needs. While no two plans are identical, your Winfield, MO physical therapist may include some combination of the following components in your carpal tunnel treatment.
1) Calming irritation and symptoms
Treatment often begins by reducing irritation to allow symptoms to ease. The goal early on is relief, not aggressive correction.
Common examples include:
- Night splinting guidance to reduce wrist strain
- Modifying activities to reduce repetitive strain
- Temporary changes to reduce strain during daily activities
- Selective use of taping techniques to support the wrist during activity
The aim is symptom relief without putting daily life on hold.
2) Mobility and movement of tendons and nerves
Improving movement through the wrist and arm involves more than the nerve alone, which is why mobility work addresses the wrist, forearm, fingers, and nearby tissues. Limited motion or stiffness anywhere along the arm can increase strain at the wrist and contribute to symptoms.
Treatment may include:
- Joint mobility techniques for the wrist and forearm to improve flexion, extension, and rotation
- Hands-on and instrument-assisted soft tissue work to address stiffness in the forearm and surrounding tissues
- Finger and thumb mobility to address stiffness or protective guarding
- Targeted tendon or nerve gliding exercises, used selectively when stiffness or sensitivity is present, such as:
- Tendon gliding: controlled finger movements (open hand, partial fist, full fist) to help the flexor tendons move more smoothly through the carpal tunnel
- Median nerve gliding: carefully guided arm and wrist movements that help the median nerve move with less irritation
- When appropriate, trigger point dry needling may be included to reduce forearm muscle tension contributing to wrist strain
These movements help reduce unnecessary strain at the wrist and allow the hand and arm to move more efficiently. These exercises are one component of care and are never used in isolation.
3) Strength, endurance, and functional training
Strengthening goes far beyond squeezing a stress ball. Treatment targets the activities you rely on daily.
This may include:
- Building grip and pinch strength in a controlled, progressive manner
- Endurance training, such as sustained holds or repeated movements, to prepare for typing, tool use, or prolonged hand activity
- Task-specific strengthening based on real-life demands
- Exercises that build tolerance to load across different wrist positions
Treatment focuses on returning to normal activities while keeping symptoms controlled.
4) Practical ergonomics that reduce strain
Simply telling someone to “sit up straight” isn’t an effective solution. Effective ergonomics looks at how small changes can reduce wrist and hand strain.
Examples may include:
- Modifying keyboard, mouse, or tool setup to keep the wrist in a more neutral position
- Lowering grip force requirements during job tasks or daily activities
- Changing task setup, height, or sequencing to limit prolonged wrist strain
Small adjustments can significantly reduce pressure on the median nerve over the course of a day. In work-related situations, advanced work rehabilitation and functional capacity evaluations may help support a safe return to job duties.
5) Use of therapeutic ultrasound when appropriate
In some cases, therapeutic ultrasound may be used as part of treatment. Application settings and dosage are selected based on the person’s specific presentation. It is not a standalone treatment and is used alongside other interventions.
6) Pre- and post-surgical rehabilitation (when needed)
Pre- and post-operative rehabilitation can play an important role in restoring hand and wrist function when surgical care is part of treatment.
Physical Therapy for Carpal Tunnel Syndrome in Winfield, MO
Axes Physical Therapy serves patients in Winfield, MO with individualized care provided by licensed physical and occupational therapists. Our Winfield, MO physical therapists average more than 15 years of experience, and our clinics offer specialized hand therapy services, including care from Certified Hand Therapists (CHTs) for complex hand and wrist conditions such as carpal tunnel syndrome.
When symptoms begin to affect sleep, work, or routine activities such as opening jars, driving, texting, or lifting, it’s time to consider a plan.
Book an evaluation with Axes Physical Therapy in Winfield, MO to clarify your diagnosis and outline a care plan that supports your goals. You can call the Axes location nearest you, request an appointment online, or come to any of our locations for a free injury screening to get started.
Carpal Tunnel Syndrome Treatment FAQs in Winfield, MO
Does typing always lead to carpal tunnel syndrome?
Typing isn’t the only cause. Many factors—including wrist position, swelling, individual anatomy, and medical conditions—can contribute to carpal tunnel symptoms.
Why do carpal tunnel symptoms flare up at night?
During sleep, the wrist may fall into bent positions and fluid redistribution can increase pressure on the median nerve. Using a wrist splint while sleeping can limit wrist bending and reduce overnight symptoms.
How do I know it’s carpal tunnel syndrome and not something else?
Diagnosis is based on your symptom pattern, physical exam findings, and, when needed, additional testing such as nerve conduction studies or EMG to confirm nerve compression or rule out other causes.
Is physical therapy effective for carpal tunnel syndrome?
Yes. Physical and hand therapy are commonly used as part of conservative care and may include mobility work, strengthening, ergonomic adjustments, and activity modifications, often alongside splinting and other symptom-management strategies.
When are injections considered for carpal tunnel syndrome?
Injections may be considered if conservative treatment hasn’t provided enough relief and temporary reduction in inflammation is needed.
When is surgery recommended?
Surgery is typically considered when conservative treatment doesn’t provide relief, symptoms are severe or long-standing, or there is concern about ongoing nerve damage.




















































































































































































