Carpal Tunnel Syndrome: Symptoms, Causes, and Treatment Options in Manchester, MO
When the median nerve is squeezed within the carpal tunnel, symptoms of carpal tunnel syndrome can begin. As nerve irritation increases, everyday hand and wrist use can become increasingly uncomfortable.
If you’re in Manchester, MO and you want a conservative, practical plan that helps you keep working and living normally and gets you back to the activities you love, focused hand therapy can be a practical place to begin. Working with experienced Manchester, MO physical therapists through Axes Physical Therapy can help support recovery while keeping life moving.
Taking the next step doesn’t have to be complicated. simply reach out to your nearest Axes clinic, book an appointment online, or visit any of our locations for a no-cost injury screening.
Quick Summary
- This condition involves compression of the median nerve in the wrist, which can result in changes in sensation, pain, and hand weakness.
- Symptoms often worsen at night and usually affect the thumb through part of the ring finger, while the little finger is typically spared.
- Symptoms are often influenced by repetitive activity, prolonged wrist positioning, swelling, and certain medical conditions.
- Providers rely on symptom patterns, exam findings, and selective nerve testing when diagnosing median nerve compression.
- Early conservative care often helps relieve symptoms and may involve splinting, activity modification, and therapeutic intervention.
- Without treatment, symptoms can progress, potentially leading to long-term nerve damage and loss of hand function.
Understanding Carpal Tunnel Syndrome
The wrist contains a narrow space known as the carpal tunnel. Small wrist bones create the base and sides of this space, with the transverse carpal ligament forming a firm roof overhead. Passing through this space is the median nerve, which originates in the neck and travels down the arm into the hand.
Increases in pressure inside the carpal tunnel, whether from swelling or other changes, can place stress on the median nerve. As a result, people may experience altered sensation and reduced strength during everyday hand tasks.
Recognizing Symptoms of Carpal Tunnel Syndrome
Carpal tunnel syndrome often starts subtly rather than with severe pain. A lot of people notice a pattern first:
Common symptoms of carpal tunnel syndrome include:
- Numbness or tingling in the thumb, index finger, middle finger, and often part of the ring finger
- Uncomfortable sensations such as burning or electric-like pain in the wrist or hand
- Nighttime symptoms, such as pain or tingling that wakes you from sleep
- Shaking the hand to reduce numbness or restore sensation
- Weakness or clumsiness in the hand, particularly during gripping or detailed tasks
- Objects slipping from the hand more often
- Discomfort originating in the wrist or hand that may radiate upward
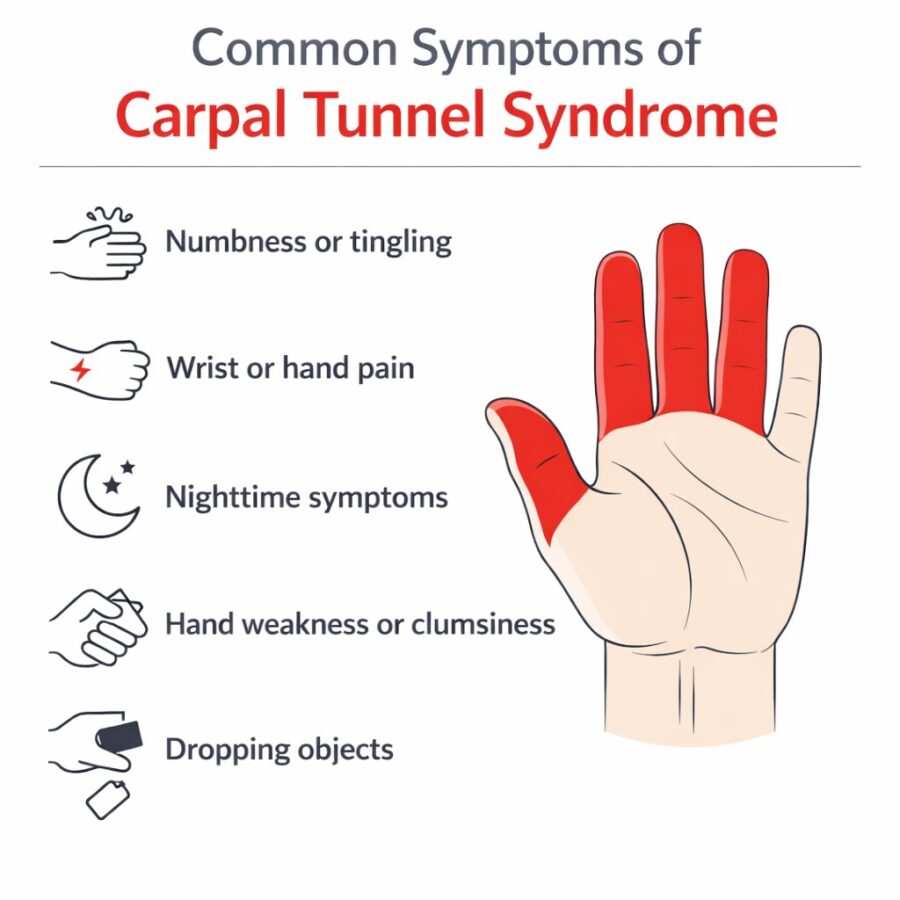
Common symptom patterns clinicians look for
In addition to the symptoms themselves, clinicians often look for specific patterns that suggest carpal tunnel syndrome:
- Symptoms that worsen at night or are noticeable first thing in the morning
- Tingling or numbness that appears during prolonged gripping or when the wrist is held in one position, like holding a phone or steering wheel
- Symptoms that briefly improve when activity stops or the wrist position changes
An important finger pattern clue
One key detail involves which fingers are experiencing symptoms. The little finger is usually unaffected in carpal tunnel syndrome since it is not supplied by the median nerve. When the pinky is involved, it can indicate that something other than carpal tunnel syndrome is contributing to symptoms.
What Contributes to Carpal Tunnel Syndrome?
In many cases, carpal tunnel syndrome develops due to several contributing factors. More often, it involves gradual pressure buildup within a confined space at the wrist.
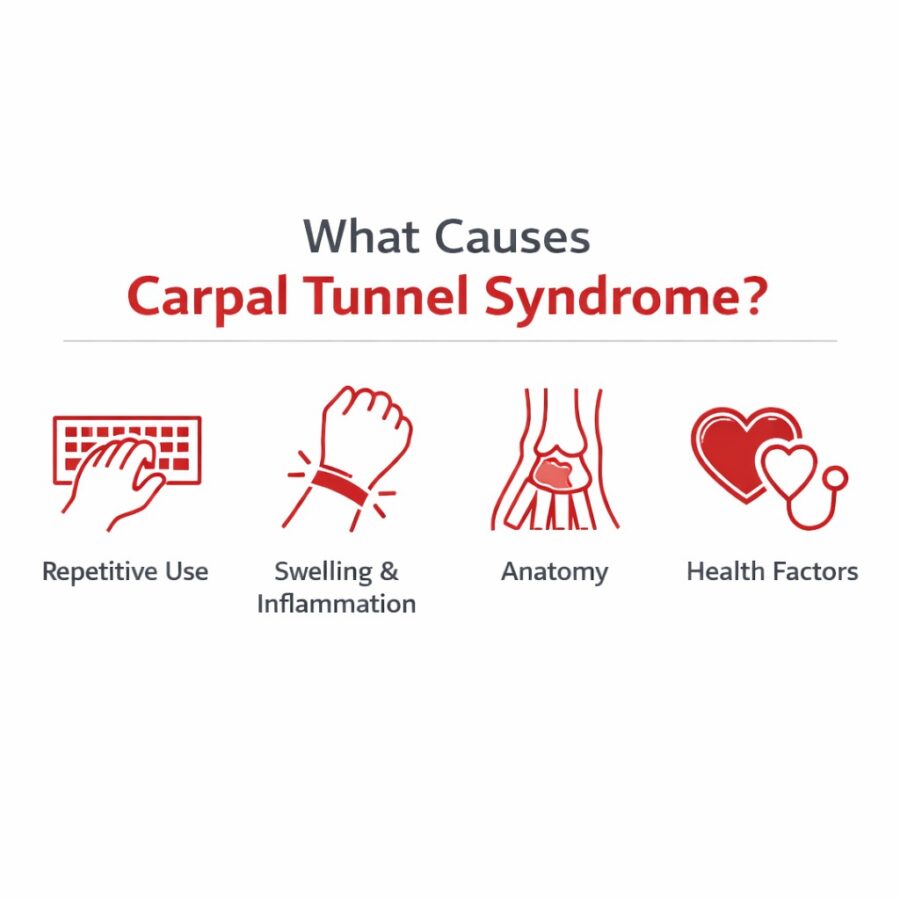
Contributing factors may include:
Ongoing wrist and hand demands
Activities that involve repetitive motions, prolonged gripping, tool use, or awkward wrist positions can increase symptoms, particularly when breaks are limited.
Wrist swelling and inflammation
Anything that increases swelling in the wrist – such as a wrist sprain or period of heavy overuse – can crowd the carpal tunnel and irritate the median nerve. Even small increases in inflammation can raise pressure in this tight space, which is why rest, icing, and wrist splinting are often effective early strategies when symptoms are mild.
Anatomical contributors
A narrower carpal tunnel or structural changes related to arthritis or trauma can increase susceptibility to symptoms.
Medical and lifestyle risk factors
Certain systemic health factors can increase the likelihood of developing carpal tunnel syndrome.
Symptoms commonly appear during pregnancy and often improve after delivery, though some individuals may remain at higher risk later on.
Smoking, excessive alcohol use, and poor diets can also contribute to the condition.
How Manchester, MO Physical Therapists Diagnose Carpal Tunnel Syndrome
Diagnosis is usually a combination of your symptom story and a physical exam, sometimes with additional testing.
The symptom pattern matters (a lot)
The diagnostic process frequently starts by looking at symptom patterns, especially nighttime symptoms and numbness triggered by prolonged gripping or wrist positioning.
Common in-office tests used during diagnosis
Physical examination often includes simple tests that assess whether specific wrist positions or light pressure bring on symptoms related to median nerve compression.
- Phalen’s test – holding the wrist in a flexed position to see if numbness or tingling develops in the fingers
- Tinel’s sign – tapping along the median nerve at the wrist to assess for tingling or shock-like sensations
- Strength testing – evaluating hand strength, including thumb muscles innervated by the median nerve
- Sensory testing – checking for reduced or altered feeling in the fingers commonly affected by carpal tunnel syndrome
Symptom patterns and exam findings are interpreted together to determine if median nerve compression is present.
When additional testing may be needed
When symptoms are unclear or more advanced, therapists may suggest further testing, such as:
- X-rays – used to evaluate bone or joint conditions like arthritis or previous fractures, rather than to diagnose carpal tunnel syndrome directly
- Ultrasound – used to view the median nerve and nearby tissues to determine whether compression is present
- Nerve conduction studies and electromyography (EMG) – helpful for evaluating nerve and muscle function when diagnosis is uncertain
When symptoms are more severe or diagnosis remains uncertain, electrodiagnostic testing is commonly used to confirm median nerve compression.
At-Home Treatment Options for Carpal Tunnel Syndrome in Manchester, MO
Most carpal tunnel treatment plans in Manchester, MO start conservatively. The focus is simple—decrease irritation to the median nerve, settle symptoms, and address contributing factors.
Immediate at-home steps for mild symptoms
Stanford suggests that if symptoms are mild, a short window of home care (1–2 weeks) may relieve symptoms, including:
- Taking breaks from symptom-provoking tasks
- Using cold packs for short intervals throughout the day
- Short-term use of NSAIDs for symptom relief
- Wearing a wrist splint to reduce pressure on the median nerve
Simple early strategies—such as more frequent breaks, avoiding aggravating activities, and cold therapy—can help calm symptoms.
How Manchester, MO Physical Therapy Treats Carpal Tunnel Syndrome
Splinting and basic advice can help, but many people need a plan that targets the underlying source of nerve irritation. That’s where physical therapy and hand therapy in Manchester, MO play an important role.
A good PT/hand therapy program in Manchester, MO often focuses on:
- Reducing nerve irritation
- Restoring wrist and forearm movement and strength
- Addressing posture and movement patterns upstream (yes, even the shoulder/neck can matter for how your arm loads)
- Helping you keep doing your job and daily tasks with less strain
What treatment may look like
Physical therapy for carpal tunnel syndrome isn’t one-size-fits-all. Plans are modified over time depending on symptom response and functional needs. Your Manchester, MO physical therapist may use a mix of the following strategies as part of treatment.
1) Calming irritation and symptoms
The early phase of treatment is centered on settling nerve irritation. This phase isn’t about pushing through pain or trying to fix everything at once.
This may involve:
- Education on night splinting to maintain neutral wrist positioning
- Activity modifications, such as changing how long or how often certain tasks are performed
- Short-term changes to ease wrist strain during routine tasks
- Short-term taping support (including Kinesio Taping®) to help reduce irritation during activity when appropriate
Care is designed to reduce symptoms without stopping normal routines.
2) Mobility and movement of tendons and nerves
Mobility work looks at movement quality throughout the wrist, forearm, fingers, and surrounding tissues, rather than focusing only on the nerve. Limited motion or stiffness anywhere along the arm can increase strain at the wrist and contribute to symptoms.
Therapy may involve:
- Joint mobility techniques for the wrist and forearm to improve flexion, extension, and rotation
- Soft tissue techniques aimed at reducing forearm muscle stiffness, including manual therapy and instrument assisted soft tissue mobilization when appropriate
- Finger and thumb mobility to address stiffness or protective guarding
- Targeted tendon or nerve gliding exercises, used selectively when stiffness or sensitivity is present, such as:
- Tendon gliding: controlled finger movements (open hand, partial fist, full fist) to help the flexor tendons move more smoothly through the carpal tunnel
- Median nerve gliding: gentle arm, wrist, and finger movements that change nerve position to reduce sensitivity and improve mobility
- In some cases, trigger point dry needling may be used to address forearm muscle tension that contributes to wrist and hand strain
Better movement through the wrist and arm helps limit unnecessary stress during daily activities. Gliding exercises are used as part of a larger plan rather than on their own and are progressed gradually.
3) Strength, endurance, and functional training
Building strength is not limited to basic hand exercises. The focus is on rebuilding tolerance for the activities you actually need to do.
Examples include:
- Gradual grip and pinch strengthening that progresses as symptoms improve
- Endurance training, such as sustained holds or repeated movements, to prepare for typing, tool use, or prolonged hand activity
- Task-specific strengthening based on real-life demands
- Training the wrist and forearm to handle load in neutral and slightly altered positions
The ultimate objective is a return to daily life without recurring symptoms.
4) Practical ergonomics that reduce strain
“Sit up straight” isn’t a plan. Ergonomics focuses on practical adjustments that limit strain on the wrist and hand.
Ergonomic changes may include:
- Adjusting keyboard, mouse, or tool positioning so the wrist stays closer to neutral
- Lowering grip force requirements during job tasks or daily activities
- Adjusting task height, setup, or order to reduce sustained wrist strain
Small adjustments can significantly reduce pressure on the median nerve over the course of a day. For occupational cases, additional work-focused rehabilitation may be used to guide return-to-duty decisions.
5) Therapeutic ultrasound when indicated
Therapeutic ultrasound may be included in certain cases as part of a treatment plan. Application settings and dosage are selected based on the person’s specific presentation. It is not a standalone treatment and is used alongside other interventions.
6) Pre- and post-surgical rehabilitation when indicated
If injections or surgery become part of the plan, pre- and post-surgical rehabilitation can help restore mobility, strength, and functional use of the hand and wrist, and support a smoother return to work and daily activities.
Carpal Tunnel Syndrome Physical Therapy in Manchester, MO
Patients in Manchester, MO receive individualized care at Axes Physical Therapy from licensed physical and occupational therapists. Clinics offer advanced hand therapy services supported by experienced therapists and Certified Hand Therapists (CHTs) for conditions involving the hand and wrist.
When symptoms begin to affect sleep, work, or routine activities such as opening jars, driving, texting, or lifting, it’s time to consider a plan.
Schedule a physical therapy evaluation with Axes in Manchester, MO to confirm what’s going on and map out a treatment path that fits your life. Get started by calling the nearest Axes location, scheduling online, or visiting any clinic for a free injury screening.
Frequently Asked Questions About Carpal Tunnel Syndrome Treatment in Manchester, MO
Does typing always lead to carpal tunnel syndrome?
Not always. While repetitive wrist and hand use can contribute, carpal tunnel syndrome is often influenced by multiple factors, including anatomy, swelling or inflammation, wrist positioning, and underlying health conditions.
What makes carpal tunnel syndrome worse during sleep?
Nighttime flare-ups often occur because wrist posture and fluid changes increase pressure in the carpal tunnel. Keeping the wrist neutral with a night splint is often helpful for managing nighttime discomfort.
How can providers tell if symptoms are carpal tunnel syndrome?
A combination of symptom patterns, examination, and selective nerve testing is used to identify carpal tunnel syndrome.
Is physical therapy effective for carpal tunnel syndrome?
Yes. Physical and hand therapy are commonly used as part of conservative care and may include mobility work, strengthening, ergonomic adjustments, and activity modifications, often alongside splinting and other symptom-management strategies.
When might steroid injections be used?
Steroid injections are sometimes used when other non-surgical treatments fail to adequately control symptoms.
When should surgery be considered for carpal tunnel syndrome?
Surgery is typically considered when conservative treatment doesn’t provide relief, symptoms are severe or long-standing, or there is concern about ongoing nerve damage.



















































































































































































