Carpal Tunnel Syndrome: Symptoms, Causes, and Treatment Options in Old Monroe, MO
Pressure on the median nerve inside the wrist can lead to carpal tunnel syndrome. As nerve irritation increases, everyday hand and wrist use can become increasingly uncomfortable.
When symptoms start interfering with everyday activities, many people in Old Monroe, MO look for a conservative place to begin, hand therapy can be an effective first step. Care guided by local physical therapists in Old Monroe, MO at Axes can help support recovery while keeping life moving.
Taking the next step doesn’t have to be complicated. you can contact the Axes location nearest you, request an appointment online, or even visit any of our locations for a no-cost injury screening.
Quick Summary
- Carpal tunnel syndrome occurs when the median nerve is compressed in the wrist, causing numbness, tingling, pain, and sometimes weakness in the hand.
- A common pattern includes nighttime symptoms that impact most fingers except the little finger.
- Symptoms are often influenced by repetitive activity, prolonged wrist positioning, swelling, and certain medical conditions.
- Providers rely on symptom patterns, exam findings, and selective nerve testing when diagnosing median nerve compression.
- Many people respond well to early, conservative care, which can include changes to activity, nighttime splinting, and physical or hand therapy.
- If left untreated, carpal tunnel syndrome may worsen over time and increase the risk of lasting nerve problems and reduced hand function.
An Overview of Carpal Tunnel Syndrome
At the wrist, the carpal tunnel forms a tight space that structures must pass through. The structure is bordered by wrist bones on the bottom and sides, with the transverse carpal ligament spanning across the top. Running from the neck through the arm and forearm, the median nerve passes through the carpal tunnel on its way into the hand.
If pressure increases within this tight space due to inflammation or structural factors, the median nerve can be affected. That’s when people start noticing changes in sensation (tingling/numbness) and sometimes weakness in tasks like gripping, pinching, or fine motor work.
Common Signs and Symptoms of Carpal Tunnel Syndrome
Symptoms of carpal tunnel syndrome don’t always appear suddenly or dramatically. For many, symptoms follow recognizable patterns early on.
Typical carpal tunnel syndrome symptoms include:
- Tingling or numbness affecting the thumb, index finger, middle finger, and sometimes part of the ring finger
- Aching, burning, or electric-type pain in the hand or wrist
- Nighttime symptoms, such as pain or tingling that wakes you from sleep
- A need to shake the hand out to “wake it up” or relieve numbness
- Weakness or clumsiness in the hand, particularly during gripping or detailed tasks
- Increased tendency to drop items
- Pain that feels like it’s coming from deep within the wrist or hand and may sometimes travel up the forearm
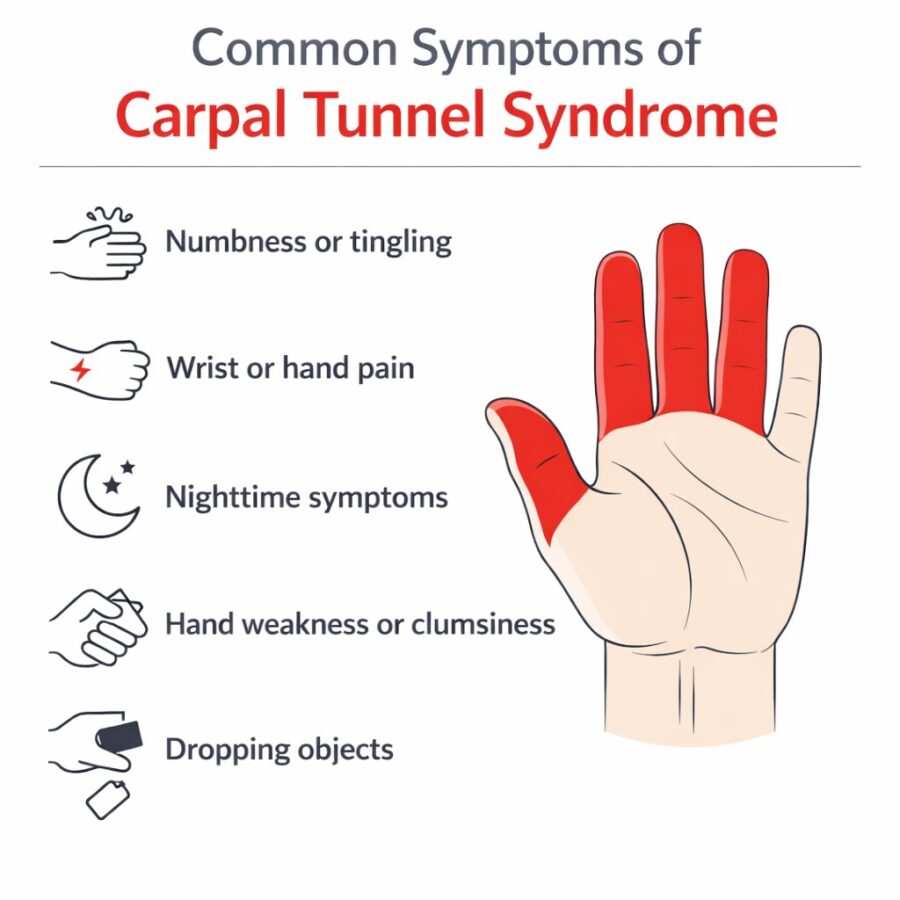
Recognizable symptom patterns
Along with reported symptoms, providers frequently assess patterns that are characteristic of carpal tunnel syndrome:
- Nighttime symptoms or numbness that’s present upon waking
- Symptoms triggered by sustained gripping or static wrist positions, including activities like reading or driving
- Symptoms that briefly improve when activity stops or the wrist position changes
A useful finger distribution clue
One important detail is which fingers are affected. The little finger is usually unaffected in carpal tunnel syndrome since it is not supplied by the median nerve. Persistent symptoms in the little finger may suggest a different nerve issue or another source of hand symptoms.
Common Causes of Carpal Tunnel Syndrome
The cause is often multifactorial rather than a single issue. In many cases, it’s not one single event; it’s pressure building over time in a tight space.
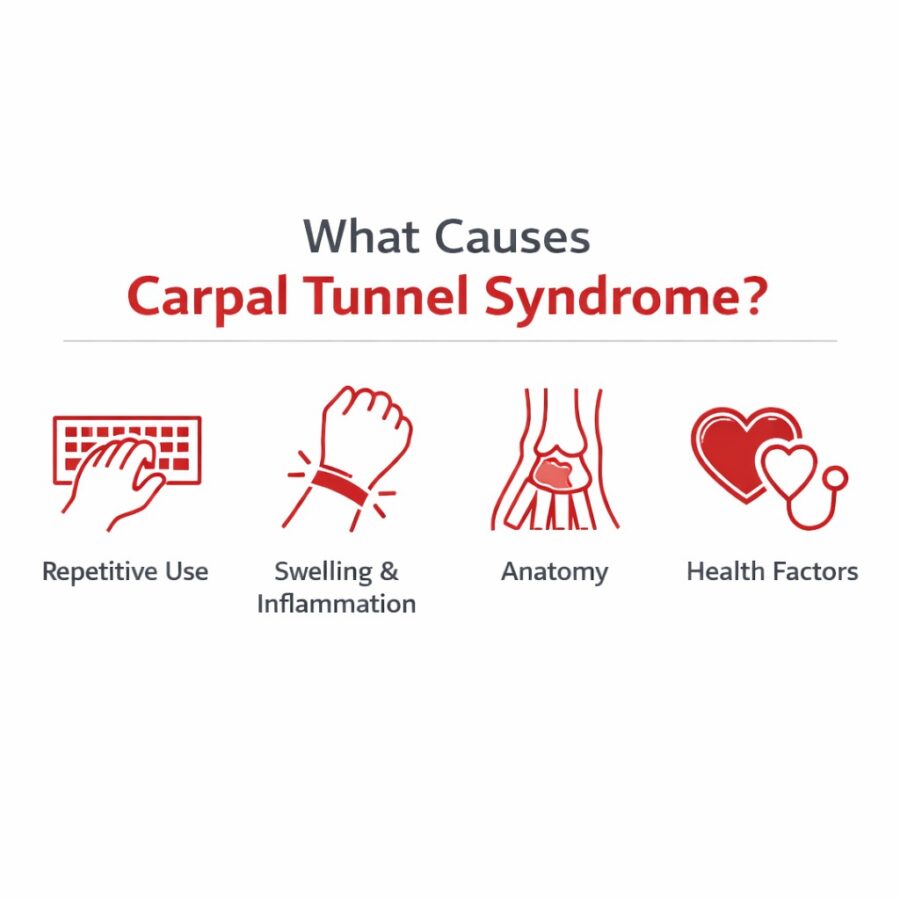
Some of the most common contributors include:
Repetitive and prolonged wrist or hand use
Typing, gripping, assembly work, tool use, and anything that keeps your wrist in awkward positions for long stretches can aggravate symptoms—especially if breaks are limited.
Swelling and inflammation
Anything that increases swelling in the wrist – such as a wrist sprain or period of heavy overuse – can crowd the carpal tunnel and irritate the median nerve. This limited space means that even minor inflammation can worsen symptoms, particularly early in the condition.
Structural and anatomical factors
Over time, arthritis or wrist injuries may alter the tunnel’s structure and increase nerve pressure.
Health and life factors that raise risk
Some health conditions are linked to increased carpal tunnel risk, including rheumatoid arthritis, diabetes, hypothyroidism, and obesity.
Fluid shifts during pregnancy can contribute to symptoms, which frequently resolve postpartum but may recur in the future.
Lifestyle factors such as smoking, heavy alcohol use, and poor nutrition may also play a role.
How Old Monroe, MO Physical Therapists Diagnose Carpal Tunnel Syndrome
Diagnosing carpal tunnel syndrome typically involves reviewing symptoms along with a hands-on physical exam, and occasionally further testing.
Why symptom patterns matter
Providers place significant weight on symptom patterns, including symptoms that worsen at night or appear during sustained wrist postures.
Physical exam tests used to diagnose carpal tunnel syndrome
As part of the physical exam, Old Monroe, MO physical therapists may perform brief in-office tests designed to reproduce symptoms linked to median nerve irritation.
- Phalen’s test – maintaining wrist flexion to check for reproduction of numbness or tingling symptoms
- Tinel’s sign – lightly tapping over the median nerve to see if tingling or electrical sensations travel into the hand
- Strength testing – assessing grip strength and thumb muscles supplied by the median nerve
- Sensory testing – assessing sensation changes in the fingers typically involved in carpal tunnel syndrome
Physical exam findings are reviewed together with symptom history to assess for median nerve compression.
Situations that call for imaging or nerve testing
In some situations, additional testing may be recommended based on symptoms and exam findings, including:
- X-rays – used to look for bone or joint issues such as arthritis or prior fracture; they are not used to diagnose carpal tunnel syndrome itself
- Ultrasound – allows visualization of nerve size and surrounding structures at the wrist
- Nerve conduction studies and electromyography (EMG) – used to assess nerve signal transmission and muscle function to confirm median nerve involvement or rule out other causes
In situations where symptoms are unclear, electrodiagnostic testing can provide definitive confirmation of nerve compression.
Managing Carpal Tunnel Syndrome at Home in Old Monroe, MO
In Old Monroe, MO, treatment for carpal tunnel syndrome usually begins with conservative care. The goal is to calm symptoms, reduce median nerve pressure, and address underlying contributors.
Steps you can take right away for mild symptoms
For mild symptoms, a short period of at-home care—often one to two weeks—may help relieve discomfort, including:
- Resting from aggravating activities
- Using cold packs for short intervals throughout the day
- Using NSAIDs to help manage pain or inflammation
- Wearing a wrist splint to reduce pressure on the median nerve
Simple early strategies—such as more frequent breaks, avoiding aggravating activities, and cold therapy—can help calm symptoms.
How Old Monroe, MO Physical Therapy Treats Carpal Tunnel Syndrome
While splints and activity advice can be useful, most cases require a more comprehensive plan. This is where physical and hand therapy become especially helpful.
An effective physical or hand therapy program in Old Monroe, MO typically emphasizes:
- Calming irritation to the median nerve
- Enhancing wrist and forearm mobility and strength
- Addressing posture and movement patterns upstream (yes, even the shoulder/neck can matter for how your arm loads)
- Allowing you to stay active and productive with less stress on the wrist
What you might do in therapy
Carpal tunnel treatment is individualized rather than one-size-fits-all. Treatment is adjusted based on symptoms, daily demands, and how the wrist and hand respond over time. While no two plans are identical, your Old Monroe, MO physical therapist may include some combination of the following components in your carpal tunnel treatment.
1) Symptom-calming strategies
Early treatment focuses on reducing irritation and giving the median nerve a chance to settle down. The goal early on is relief, not aggressive correction.
Common examples include:
- Night splinting guidance to reduce wrist strain
- Modifying activities to reduce repetitive strain
- Short-term changes to ease wrist strain during routine tasks
- Short-term taping support (including Kinesio Taping®) to help reduce irritation during activity when appropriate
Care is designed to reduce symptoms without stopping normal routines.
2) Mobility and movement of tendons and nerves
Mobility-focused treatment examines how the wrist, forearm, fingers, and surrounding structures move together, not just the median nerve. When motion is limited along the arm, added strain may show up at the wrist and worsen symptoms.
Therapy may involve:
- Wrist and forearm joint mobility to improve bending, straightening, and rotation
- Hands-on and instrument-assisted soft tissue work to address stiffness in the forearm and surrounding tissues
- Improving finger and thumb movement to address protective stiffness
- Selective use of tendon or nerve gliding exercises when stiffness or sensitivity is identified, including:
- Tendon gliding: specific finger positions such as open hand, partial fist, and full fist to encourage smoother tendon movement through the carpal tunnel
- Median nerve gliding: controlled movements designed to improve nerve mobility and reduce sensitivity
- For some individuals, dry needling may be used to address muscle tension that increases stress on the wrist and hand
These movements help reduce unnecessary strain at the wrist and allow the hand and arm to move more efficiently. Gliding exercises are used as part of a larger plan rather than on their own and are progressed gradually.
3) Strength, endurance, and functional training
Strengthening goes far beyond squeezing a stress ball. The emphasis is on restoring tolerance for real-world demands.
Examples include:
- Gradual grip and pinch strengthening that progresses as symptoms improve
- Endurance-focused exercises to prepare for prolonged hand use, including typing or tool work
- Functional strengthening, including lifting, carrying, pushing, or pulling tasks that mimic work or daily demands
- Exercises that build tolerance to load across different wrist positions
The goal is to help you return to daily activities without symptoms flaring back up.
4) Practical ergonomics that reduce strain
“Sit up straight” isn’t a plan. Ergonomics is about making realistic changes that reduce unnecessary strain on the wrist and hand.
Ergonomic changes may include:
- Adjusting keyboard, mouse, or tool positioning so the wrist stays closer to neutral
- Reducing grip force demands during work or daily tasks
- Modifying how tasks are performed to minimize prolonged wrist stress
Small changes made consistently can help limit pressure on the median nerve. For occupational cases, additional work-focused rehabilitation may be used to guide return-to-duty decisions.
5) Therapeutic ultrasound (when appropriate)
Therapeutic ultrasound may be included in certain cases as part of a treatment plan. Application settings and dosage are selected based on the person’s specific presentation. Ultrasound is combined with other treatment strategies rather than used on its own.
6) Rehabilitation before and after surgery, when appropriate
If injections or surgery become part of the plan, pre- and post-surgical rehabilitation can help restore mobility, strength, and functional use of the hand and wrist, and support a smoother return to work and daily activities.
Carpal Tunnel Syndrome Physical Therapy in Old Monroe, MO
Axes Physical Therapy serves patients in Old Monroe, MO with individualized care provided by licensed physical and occupational therapists. Our team brings over 15 years of experience on average and includes access to specialized hand therapy, with Certified Hand Therapists (CHTs) available for complex wrist and hand conditions.
If hand or wrist symptoms are disrupting sleep, job duties, or simple daily tasks, getting a clear plan can make a difference.
Schedule a physical therapy evaluation with Axes in Old Monroe, MO to identify the source of symptoms and build a plan that works for your daily life. You can call the Axes location nearest you, request an appointment online, or come to any of our locations for a free injury screening to get started.
Common Questions About Carpal Tunnel Syndrome Treatment in Old Monroe, MO
Is typing the main cause of carpal tunnel syndrome?
Although typing is commonly blamed, carpal tunnel syndrome typically develops due to a combination of factors rather than a single activity.
Why is carpal tunnel syndrome worse at night?
During sleep, the wrist may fall into bent positions and fluid redistribution can increase pressure on the median nerve. Using a wrist splint while sleeping can limit wrist bending and reduce overnight symptoms.
How do I know it’s carpal tunnel syndrome and not something else?
Providers rely on symptom history, physical exam findings, and sometimes nerve testing to confirm carpal tunnel syndrome or exclude other conditions.
Does physical therapy work for carpal tunnel symptoms?
Many people benefit from physical or hand therapy as part of a conservative treatment plan for carpal tunnel syndrome.
When do injections make sense?
Steroid injections are sometimes used when other non-surgical treatments fail to adequately control symptoms.
At what point is surgery an option?
Surgical treatment may be recommended if symptoms are persistent, severe, or continue to worsen despite conservative care.



















































































































































































